Topics
Get the Latest News and Insights From MHQP
Sign up for our emails for access to our initiative announcements, insights, and informative data.
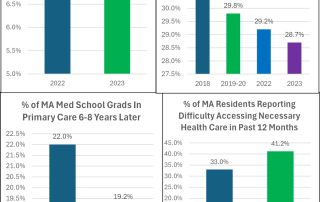
The Primary Care Dashboard Paints a Troubling Picture for Massachusetts Healthcare
By Barbra G. Rabson
(June 2025)
“We’re beyond a crisis.”
That is how State Senator Cindy Friedman chose to characterize the current state of primary care in the Commonwealth in her opening remarks to Massachusetts’ newly established Primary Care Access, Delivery, and Payment Task Force in April.
The updated data in the Primary Care Dashboard released last week by the Center
Expanding MHQP’s Impact: Insights and Opportunities in Behavioral Health
(January 2025)
MHQP’s Board of Directors has recommended an expansion in MHQP’s work scope to include primary care-adjacent clinical areas, particularly behavioral health. The Board sees a critical need for MHQP’s measurement expertise and sense-making capabilities in this space, given behavioral health’s significant impact on physical health and overall healthcare costs. This need has become even more urgent given
Lessons from Steward and the Need for Primary Care Reform in Massachusetts
(May 2024)
 Barbra Rabson and Katherine Gergen Barnett have collaborated again, this time on a commentary in Perspectives in Primary Care, published by the Harvard Medical School Center for Primary Care. The opinion piece, entitled “Lessons from Steward and the Need for Primary Care Reform in Massachusetts,” traces the roots of
Barbra Rabson and Katherine Gergen Barnett have collaborated again, this time on a commentary in Perspectives in Primary Care, published by the Harvard Medical School Center for Primary Care. The opinion piece, entitled “Lessons from Steward and the Need for Primary Care Reform in Massachusetts,” traces the roots of
Unsustainable: An Honest Assessment of Massachusetts’ Healthcare Performance
By Barbra G. Rabson
(July 2023)
 Last month, the Commonwealth Fund published its annual scorecard on state health performance and gave Massachusetts the top overall ranking. The ranking was based on several metrics collected in 2019, 2020 and 2021 covering seven categories ― Reproductive and Women’s Health, Access and
Last month, the Commonwealth Fund published its annual scorecard on state health performance and gave Massachusetts the top overall ranking. The ranking was based on several metrics collected in 2019, 2020 and 2021 covering seven categories ― Reproductive and Women’s Health, Access and
MHQP Celebrates Barbara Spivak and Julita Mir
(November 2022)
MHQP is pleased to celebrate the invaluable contributions of two members of our Board of Directors, Barbara Spivak, MD, and Julita Mir, MD, both of whom have an enormous impact on MHQP’s strategy and direction.
Barbara Spivak, MD
 A primary care provider and President and CEO of the Mount Auburn Cambridge
A primary care provider and President and CEO of the Mount Auburn Cambridge
Employee Spotlight: Raji Rajan
(November 2022)
 Raji Rajan, MBA, MS, and her husband, Raj, both decided to shift their careers to work in healthcare after the medical procedure that saved Raj’s life. This was back in 2008. Raji was spending her days working as a Senior Software Engineer at Fidelity and her evenings helping Raj
Raji Rajan, MBA, MS, and her husband, Raj, both decided to shift their careers to work in healthcare after the medical procedure that saved Raj’s life. This was back in 2008. Raji was spending her days working as a Senior Software Engineer at Fidelity and her evenings helping Raj
Evaluating Patient Experiences of Primary Care by Visit Mode and Visit Reason During the Pandemic
(September 2022)
 MHQP’s Jim Courtemanche, Nathalie McIntosh, Raji Rajan and Barbra Rabson co-authored, along with Blue Cross Blue Shield of Massachusetts’ Mark Friedberg, an important study investigating adult patient experiences of, and satisfaction with, in-person, video, and telephone visits in primary care during the COVID-19
MHQP’s Jim Courtemanche, Nathalie McIntosh, Raji Rajan and Barbra Rabson co-authored, along with Blue Cross Blue Shield of Massachusetts’ Mark Friedberg, an important study investigating adult patient experiences of, and satisfaction with, in-person, video, and telephone visits in primary care during the COVID-19
Employee Spotlight: Natalya Martins
 (August 2022)
(August 2022)
Natalya Martins, MPH, has a placard with a quote from Indigenous Australian and activist Lilla Wilson hanging in her office:
“If you have come here to help me you are wasting your time, but if you have come because your liberation is bound up with mine, then let us work
It’s Time to Better Understand and Address Disparities in Patient Experiences
By Barbra G. Rabson
(July 2022)

The pandemic has shown us that we are not doing enough to equally promote health for people of all races and ethnicities. Given that there are well-known and researched disparities across all aspects of care, it may not surprise you to learn that Black, Hispanic and Asian
Backlash Must Fuel Renewed Commitment to Health Equity
By Barbra G. Rabson
(February 2022)

Since the summer of 2020, when the murder of George Floyd and the COVID pandemic spawned a reawakening about racial injustice in this country, I have been impressed and proud of the commitment to health equity at so many levels in the Massachusetts healthcare system. Company CEOs,
Patients Really Like Telehealth. Let’s Resolve to Make It Work.
By Barbra G. Rabson
(January 2022)
 At the beginning of the pandemic, I penned a post I called “Now Is the Time to Get Telehealth Right” in which I suggested that something good might emerge from what I called our “grand telehealth experiment.” Well, my friends, the pandemic may not be over
At the beginning of the pandemic, I penned a post I called “Now Is the Time to Get Telehealth Right” in which I suggested that something good might emerge from what I called our “grand telehealth experiment.” Well, my friends, the pandemic may not be over
It’s Time We Started Collecting Data on People with Disabilities
By Barbra G. Rabson
(December 2021)
 As a measurement organization, MHQP has a long track record for reporting comparative performance information to drive improvements in Massachusetts healthcare. We are now focused on reporting performance on health equity and are working to generate the data to enable us to do so. MHQP and our
As a measurement organization, MHQP has a long track record for reporting comparative performance information to drive improvements in Massachusetts healthcare. We are now focused on reporting performance on health equity and are working to generate the data to enable us to do so. MHQP and our
Are Severe Staffing Shortages the “Long COVID” for the Healthcare System?
By Barbra G. Rabson
(October 2021)
 COVID-19 has disrupted our healthcare system in unimaginable and incalculable ways. While we hope that we may soon emerge from the intense burden created by the crisis, the long-lasting impacts of the pandemic are just beginning to come into focus. One of these long-lasting impacts – an
COVID-19 has disrupted our healthcare system in unimaginable and incalculable ways. While we hope that we may soon emerge from the intense burden created by the crisis, the long-lasting impacts of the pandemic are just beginning to come into focus. One of these long-lasting impacts – an
The Value of Primary Care: How Come They See It and We Don’t?
By Barbra G. Rabson
(July 2021)

In May, the National Academy of Science, Engineering and Medicine (NASEM) issued an important new report called Implementing High-Quality Primary Care: Rebuilding the Foundation of Health Care. It received very little attention.
This was extremely worrisome for us at MHQP because, as an organization that has been measuring
Primary Care’s Value Proposition and the Damage Done by the Pandemic
By Barbra G. Rabson
(April 2021)
 MHQP has been measuring and publicly reporting about quality and patient experiences in primary care for nearly two decades. Never before have I known a moment such as this when I worry for the future of primary care in our state.
MHQP has been measuring and publicly reporting about quality and patient experiences in primary care for nearly two decades. Never before have I known a moment such as this when I worry for the future of primary care in our state.
MHQP first began to investigate the health
From Pandemic Fix to Permanent Fixture: How to Ensure Telehealth Lives Up to Its Full Potential
By Barbra G. Rabson
(November 2020)
Telehealth utilization quickly soared in Massachusetts in the early days of the pandemic, not just because it filled an obvious need as a way for providers and patients to connect when face-to-face interactions were not possible, but also because Governor Baker issued an order requiring insurers to
it filled an obvious need as a way for providers and patients to connect when face-to-face interactions were not possible, but also because Governor Baker issued an order requiring insurers to
Meeting the Moment in Telehealth
By Barbra G. Rabson
(August 2020)
When asked what they have learned about themselves as a clinician using telehealth in a recent MHQP survey, one physician responded, “We are an incredibly versatile lot. Our commitment to lifelong learning and constant change in our profession has trained us well for meeting this moment successfully.”
MHQP survey, one physician responded, “We are an incredibly versatile lot. Our commitment to lifelong learning and constant change in our profession has trained us well for meeting this moment successfully.”
“Meeting
Listen Up, America. Now is the Time to Address Racism in our Healthcare System
by Brittney Gedeon, Rising Junior and Presidential Scholar at Boston College and MHQP Summer Intern
(June 8, 2020)
The senseless death of George Floyd at the hands of four police officers in Minneapolis has shocked and outraged millions of people throughout the country. As a nation, we should condemn the racial injustices we see in policing and
Now Is the Time to Get Telehealth Right
By Barbra G. Rabson
(April 2020)
 Amid all the horror and hardship of the COVID-19 pandemic, maybe something good will emerge on the other side of it for the healthcare system. Now is our chance to finally get telehealth right.
Amid all the horror and hardship of the COVID-19 pandemic, maybe something good will emerge on the other side of it for the healthcare system. Now is our chance to finally get telehealth right.
Before the pandemic struck, MHQP was working with a distinguished panel of experts to
The Future of Primary Care in Massachusetts
By Barbra G. Rabson
(October 2019)
Lately, I’ve been thinking a lot about the future of primary care in Massachusetts. I was  inspired in part by work we’ve been doing at MHQP to explore barriers to affordability through the patient’s eyes, and lack of access to primary care was one of those
inspired in part by work we’ve been doing at MHQP to explore barriers to affordability through the patient’s eyes, and lack of access to primary care was one of those
The Link Between Patient Experience and Affordability: The Potential Power of Patients
 By Barbra G. Rabson
By Barbra G. Rabson
(May 2019)
I’ve spent the last two decades of my career dedicated to measuring and improving patient experience and patient engagement and have always believed that listening to patients about their experiences can be our best path to improving our healthcare system. Recently, I’ve had the opportunity to see