Clinical Quality Data Continue to Uncover Disparities in Primary Care Services
(April 2026)

Clinical quality performance data that MHQP has collected and aggregated from participating commercial payers under contract with the Center for Health Information Analysis (CHIA) reveal statewide disparities in key primary care services. CHIA published these data in March in its Annual Report on the Performance of the Massachusetts Health Care System.
While MHQP has documented disparities in patients’ reported experiences for several years, the recent stratification of clinical quality data provides additional insight into disparities in the delivery of essential services and clinical outcomes such as cancer screenings, diabetes management, and pediatric care.
The data below reveal disparities across all 5 care domains — behavioral health, chronic conditions, maternity care, pediatrics, and preventive care — when comparing Black/African American and Asian patients to White patients and Hispanic patients to non-Hispanic patients. By bringing these disparities into public view, MHQP aims to support transparency, highlight areas for improvement, and help ensure that all Massachusetts residents receive high-quality care equitably.
Scores for Black patients were significantly worse than for White patients on 9 of the 17 measures. Scores for Asian patients were significantly worse than White patients for 4 measures and significantly better for 3 measures. Scores for Hispanic patients were significantly worse than for Non-Hispanic patients on 7 of the 17 measures.
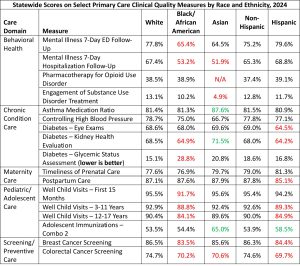
Note: figures in red and green are statistically significant for Black/African American patients and Asian patients versus White patients and for Hispanic patients versus Non-Hispanics patients; red means worse and green means better.
“These findings show that disparities in primary care are not just anecdotal — they are measurable and happening across essential services that patients rely on every day,” said MHQP President and CEO Barbra Rabson. “By bringing attention to these disparities, we hope to spur continued action across the health care system to advance more equitable delivery of high-quality care for all patients in Massachusetts.”
These data represent care provided to commercially-insured patients in 2024, based on HEDIS® data aggregated across five Massachusetts health plans. HEDIS (the Healthcare Effectiveness Data and Information Set) is a comprehensive set of standardized performance measures designed to provide purchasers and consumers with the information they need for reliable comparison of provider performance.*
Patients can review information about the performance of medical practices in their community on these measures on MHQP’s consumer-facing website, www.healthcarecompassMA.org, offering them a way to compare and contrast provider groups in their service area.
————-
*HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA).

