2023 MHQP Clinical Guidelines Highlight the Impact of Systemic Racism on Health Outcomes
 (April 2023)
(April 2023)
“Patients may be more likely to develop type 2 diabetes if they are Black, Alaska Native, American Indian, Asian, Native Hawaiian, Pacific Islander, or Hispanic/Latino.”
This was one of the “Risk Factors for Type 2 Diabetes” identified in the Diabetes section of last year’s version of MHQP’s Clinical Guidelines. MHQP revises these evidence-based, best practice recommendations each year to ensure all patients throughout Massachusetts receive up-to-date standards of care.
The statement is true, but it doesn’t tell the whole story.
“Race is a social construct without biological meaning,” explains Natalya Martins, MPH, MHQP’s VP of Programs, who has overseen the process of revising MHQP’s Clinical Guidelines for the past few years. “There are multiple dimensions of risk factors at play here.”
To address this issue, the 2023 version of the Guidelines, released by MHQP this week, explicitly draws attention to the fact that social determinants of health intersect with racism to impact health outcomes.
“We appreciate MHQP’s leadership in undertaking this critically important work to incorporate the impact of racism on health outcomes into these guidelines because we know Boston residents of color suffer higher morbidity and mortality from several chronic conditions and cancers,” says Dr. Bisola Ojikutu, Commissioner of Public Health and Executive Director of the Boston Public Health Commission. “This approach allows clinicians to more fully understand all aspects of risk in the delivery of clinical care for each patient.”
Beyond Race as the Driver
That same guidance in the new 2023 version of the Guidelines provides much broader context:
“Diabetes and pre-diabetes prevalence varies among racial and ethnic groups, with the highest rates among American Indian and Alaska Native patients, then Black patients, then Hispanic/Latino patients, then Asian patients, and with the lowest rates among White patients (CDC, 2022). These differences are likely due to complex interactions of social determinants of health, including access to healthy and affordable foods, access to safe, affordable, and accessible physical activity options, access to health care, education about diet and exercise as prevention tools, socioeconomic status, and access to affordable and equitable medical care.”
2022 Adult Guidelines Diabetes Section: 2023 Adult Guidelines Diabetes Section:
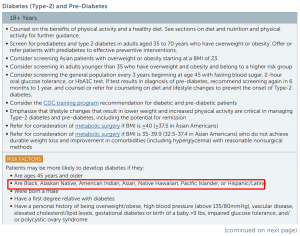
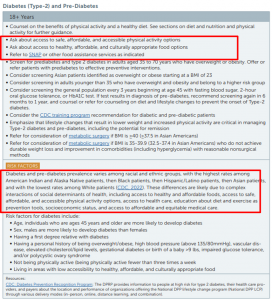
Convening Experts
MHQP executed this and other changes under the guidance of workgroups of clinical advisors and health equity experts from participating organizations convened by MHQP to review language and recommend revisions. These advisors helped MHQP determine the best ways to incorporate race and other unmodifiable patient risk factors into the Guidelines.
Based on the advice of Dr. Ojikutu and the other members of the advisory workgroups, MHQP made the following key changes to the Guidelines this year:
- A new section on Racism, Discrimination, and Health which provides information on the impact of racism and other forms of discrimination on health, includes primer definitions for systemic, interpersonal, and internalized racism, and discusses the relationship between racism, chronic stress, and health outcomes.
- Narratives that place race and ethnicity as risk factors in the context of complex interactions of access to healthcare and other social determinants of health. This strategy is also employed when considering other unmodifiable risk factors, like gender identity and sexual orientation.
- Caveat language to emphasize that race is social construct, not based in biology, when race was included in a calculation for disease risk.
- Solutions-oriented action statements/recommendations, where appropriate, to address upstream determinants of health.
“Pointing to race as a risk factor masks the role of the structural causes of health disparities and impedes progress towards health equity,” says Martins. “We hope this approach helps providers address the impact of racism and other forms of discrimination on health.”
Please click HERE to learn more about how to access MHQP’s Clinical Guidelines for your organization.

